Advanced Herbal Support for Coughs and Congestion Leave a comment
By Kat Wright, M.A.
Coughing is one of the most obvious and indisputable signs of human illness. In addition to being the main cause for patient visits to doctors, over a billion dollars are spent each year on over-the-counter (OTC) cough remedies in the US. With so many people filling medical clinics and spending so much money seeking relief from this common malady, one wonders why the persistent sounds of sick, coughing people remains such a defining feature of Winter.
The answer is that most cold and flu treatments are designed to suppress the symptoms of cough, and do nothing to address the cause. As Dr. Jake Fratkin points out, even the American College of Chest Physicians (ACCP) has noted that OTC cough expectorants and suppressants don’t treat the underlying causes of the cough, and often don’t do much to help relieve symptoms.
Additionally, the conventional medical practice of giving antibiotics to patients for colds and flu has been shown to be completely ineffective, since antibiotics only work against bacteria, not viruses, and roughly 95 percent of all coughs are caused by viruses.
And though antibiotics may slow down the production of mucus, they can weaken the immune system and contribute to the proliferation of deadly antibiotic-resistant forms of bacteria. What is really needed is a safe and effective way of targeting the viruses that cause us to cough.
Understanding Why You Cough
Contrary to popular belief, coughing is not the body’s primary mechanism for expelling phlegm from the body. Think about what happens when you take a cough expectorant. You stop coughing. And what happens to all of the mucus and phlegm in your chest that was making you so miserable? As Professor Alyn H. Morice, of Castle Hill Hospital in East Yorkshire, England explains it, “there is little reason to suggest that the coughing associated with an upper respiratory tract infection serves any use for the body. While a small amount of mucus may be expectorated (ejected through the mouth), in no way does coughing contribute to a significant clearing of the airways in normal subjects.
If one looks at an extreme example of infectious airway inflammation, such as community acquired pneumonia, despite the sometimes extensive production of mucus and phlegm, the vast majority of material is removed by phagocytosis,” (a process wherein the body absorbs the mucus and phlegm from the respiratory system and sends it via the bloodstream to the liver and the kidneys to be cleaned-up and excreted).
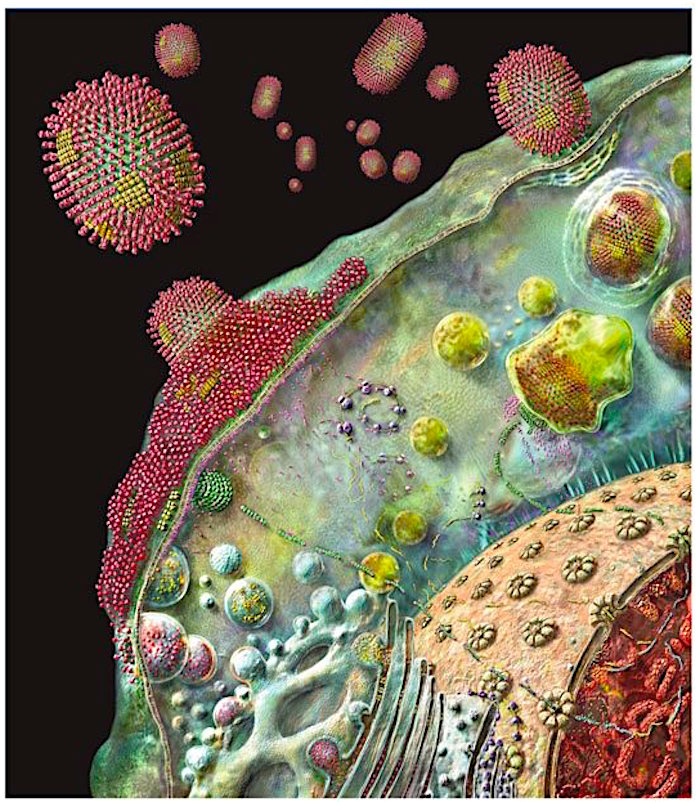 |
| Fig. 1. At upper right, a virus particle lands on a cell surface and taken into the cell. The genetic information of the virus enters the cell and heads for the nucleus where it directs production of new viral components. As these collect at the cell surface they form new viruses which then bud from the cell to be released to spread out and infect additional cells. |
So if coughing isn’t an effective means of clearing our lungs when we’re sick, what exactly causes us to cough so uncontrollably when we come down with a cold or flu?
As it turns out, coughing is a highly sophisticated biological trick developed by viruses to help them to spread to new hosts.
To understand how this works, it is important to note that while bacteria can reproduce by cell division, viruses are unable to reproduce on their own. To get around this viruses have learned how to get their infected hosts to do the work for them. First, a microscopic viral particle has to gain entry into a healthy cell in a host (Fig. 1 above). Once inside a cell the virus hijacks the internal reproductive machinery and reprograms it with new instructions that force the cell to produce multiple copies of the original virus. Eventually the cell swells and releases millions of new copies of the original virus back into the host. And this is the point where the virus employs another clever trick to spread the newly hatched viral particles to a new host. It forces you to start coughing.
How Viruses Hijack the Human Cough Reflex
Research reveals that viruses take advantage of a basic biochemical mechanism to force their hosts to cough. Coughing is a powerful nervous reflex that is normally controlled by airway receptors that line the human respiratory system. These specialized receptors, called vanilloid receptors, react to pressure or chemical stimuli to trigger a cough. Large numbers of vanilloid receptors are found in the upper portion of the respiratory tract, especially at the top of the tract in the throat and larynx (Fig. 2). As one moves down the respiratory tract and into the bronchial tubes, the number of these receptors steadily declines until, deep in the lungs, there are no more vanilloid receptors.
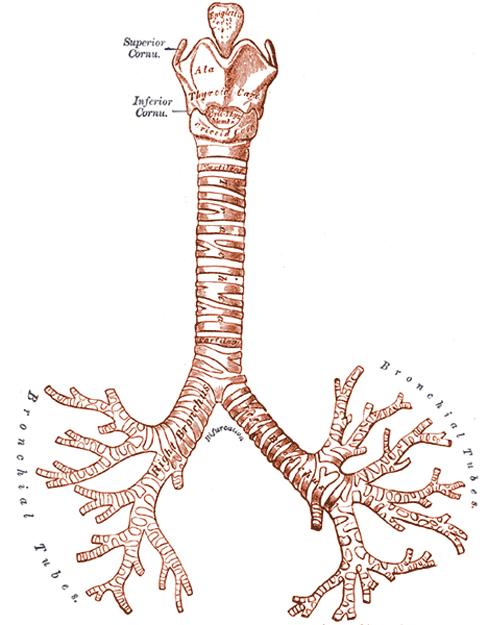
In the process of infecting a new host, some of the viruses attach to the vanilloid receptors. Doing so stimulates the immune system and causes it to launch a defensive inflammatory response that results in coughing. By activating this immune response and triggering the cough reflex, the virus has effectively turned one of the body’s primary defense systems into a highly efficient tool for spreading infection. Considering that a typical cough can propel millions of viral particles out of the body at close to the speed of sound, coughing is an impressively efficient method of spreading disease.
As Professor Morice points out, “It makes perfect sense for respiratory viruses and bacteria to have evolved the ability to cause cough. Once an organism has successfully invaded the respiratory tract its main problem for continued survival is how to spread to the next host. Some viruses do this by triggering inflammation and producing intense amounts of mucus to manually transmit themselves from person to person with infected secretions. However, the majority of viruses are required to transmit themselves in aerosolized droplets.”
In other words, coughing is a simple act of biochemical trickery that allows viruses to take over and control a basic human reflex to spread from a single host to many others.
Right Receptor, Wrong Place
If you’ve ever wondered why you catch a cold or flu while others around remain healthy, the fault may be with your receptors. As it turns out, the location and type of vanilloid receptors each person possesses plays a significant role in the development and outcome of a viral infection.
While some people possess receptors that make them susceptible to certain strains of viruses, others don’t.
And even when people have the right receptors for a specific virus, if those receptors are located too far down in the respiratory tract, the viruses may not survive long enough to penetrate deep enough to cause harm.
The importance of receptor location in the outcome of viral infections became clear after scientists examined a number of individuals who died after becoming infected with the H5N1 bird flu. In their research the scientists discovered that each of the victims possessed receptors in their throats and trachea that were susceptible to the specific H5N1 viral strain involved in the outbreak. Others in the same community who were exposed to H5N1 in an identical manner remained free of the disease because they lacked the right receptors in their throats and trachea, thereby preventing the virus from gaining a toehold and migrating deeper down into their lungs.
Feeling Better, Yet Still Coughing?
Ever wonder why you are still coughing weeks after you’ve begun to feel better? Consider this: while your immune system can defeat a typical viral infection in about 4 to 5 days, the inflammatory immune response can persist long after the virus is gone. In the process of killing off the primary infection the immune system responds by releasing a massive cascade of cytokines (inflammatory agents) to destroy the invading pathogens. If the immune response overreacts as with SARS and H5N1 the attack can further damage and irritate lung tissues, leading to a prolonged cough that can last for weeks, or even months, after the infection has been resolved.
Unfortunately, according to Dr. Fratkin, “Western medicine has very little to offer those suffering viral infections of the upper respiratory tract, such as colds and influenza. Classical and Modern Chinese herbal medical literature, on the other hand, documents over 50 herbs that exhibit strong anti-viral effects. It is unfortunate that the general public in the United States is largely unaware of this extraordinary treasure-chest of Chinese herbs and herbal products that effectively address common viruses.”
History of BronchoPhase Development
Dr. Fratkin maintains a busy clinical practice in Boulder, Colorado where he specializes in internal disorders, infections and pediatrics. Since becoming a doctor of Oriental Medicine in 1978, Dr. Fratkin has also served as a teacher, department chair, and author, while lecturing extensively on Chinese herbal medicine and nutritional medicine to advanced practitioners around the country.
I asked Dr. Fratkin to discuss the development of BronchoPhase. “This formula is the result of my clinical experience, as well as my training in the respiratory department of the Xi Yuan TCM Hospital in Beijing, China. I first created this particular formula 12 years ago, and it is one of the two most popular formulas I use, based on the number of people we give it to.”
Dr. Fratkin explained that, according to Traditional Chinese Medicine (TCM), there are seven distinct stages, or presentations, of cough. The first indications of infection reveal where the virus has entered the body, i.e., sore throat, nasal congestion, and/or cough.
For many people the first symptom is usually a sore throat. The more severe the pain, the more likely the infection is going to develop into a cough. In the next stage, as the virus moves from the initial site of infection and migrates into other areas of the body, additional symptoms begin to show up, such as nasal infection or deep congestion in the chest.
According to Dr. Fratkin, it is important to take prompt, aggressive action during the first stages before the problems has a chance to spread.
“The stage that BronchoPhase addresses includes both Lung Fire (strong barking cough without phlegm, seen in croup) and Phlegm Heat (production of yellow phlegm). This type of coughing is common throughout the year, and is aggravating enough to bring people to the clinic, where otherwise they would have “waited it out.” In this stage of cough, there is a lot of heat in the lungs, and phlegm production is small or sticky (rather than profuse and copious). Cough is frequent, the lungs hurt, and there may be coughing at night. This stage can last from 2 to 10 days without herbal treatment.”
By combining herbs traditionally used in different formulas, BronchoPhase is particularly useful for addressing the root causes of cough due to its ability to 1) address the microbial origins of cough, and 2) gently normalize the immune over-reaction to resolve the inflammatory aftermath.
BronchoPhase Herbs
BronchoPhase relies on classical formulas, some dating back to the 15th century, that remain popular today and continue to be used by millions of people throughout Asia. Significantly, a growing body of scientific research has shed light on properties of traditional herbal ingredients in BronchoPhase that have historically used to support lung health.
• Andrographis (Chuan Xin LIan, Andrographis Paniculata) is a safe traditional botanical for supporting upper respiratory tract health per analysis of seven double-blind controlled trials.1 Andrographis has been shown to inhibit RANTES (Regulated upon Activation normal T-cell Expressed and Secreted) in inflamed bronchial cells.2 RANTES is a chemoattractant for eosinophils, monocytes and lymphocytes that is stored in, and released by, platelets and activated T-cells. In related research, andrographolide, an active ingredient in Andrographis, has been shown to be responsible for the herb’s inflammatory modulating actions, including the reduction of cytokine and peritoneal deposition of neutrophils, and modulation of lung inflammation in vivo.3 Extracts of Andrographis exhibit potent inflammatory modulating and antioxidant actions in mouse models.4
• Scutellaria (Huang Qin, Radix Scutellaria Baicalenses) has a long history of use in Traditional Chinese Medicine to support a healthy immune system.5,6 In related research, baicalein, a major flavonoid in Scutellaria, has been shown to support cardiovascular health.7 Research also shows that Scutellaria modulates inflammatory activity of nitric oxide (NO), cytokine, chemokine and growth factor production in macrophages,8 as well as inhibiting histamine and leukotriene release.9
• Gardenia Jasminoides (Zhi Zi, Gardenia Jasminoides) contains genipen, an active ingredient that has been shown to regulate inflammatory activity in mice.10 Another ingredient, geniposide, has been shown to enhance levels of glutathione, an important immune system amino acid that helps determine modulation of immune response, including cytokine production, in animal models.11
• Morus Alba (Sang Bai Pi, Radicis Cortex Morus Alba) extracts have been shown to modulate mast cell degranulation and histamine release.12 In one study, a polysaccharide from Morus root has been shown to have immune-modulating activity.13
• Belamcanda (She Gan, Rhizoma Belamcandae Chinensis) contains an active ingredient, irigenin, that has been shown to possess inflammatory modulating properties in macrophage immune cells.14
• Asparagus (Tian Men Dong, Asparagus Cochinchinensis) extracts have been shown to modulate inflammatory actions.15
• Trichosanthes (Gua Lou Ren, Semen Trichosanthes) extracts contain inflammatory regulating ingredients, including triterpenes.16
• Fritillaria (Chuan Bei Mu, Bulbus Fritillaria Chirrhosa) is considered an anti-tussive herb, with imperialine identified as the major bioactive component.17
• Platycodon (Jie Geng, Radix Platycodon Grandiflorum) is widely used in Chinese herbal medicine for upper respiratory issues. Active ingredients platycodon D and D3 increase mucin release in rat and hamster tracheal cells and provide useful expectorant effects.18 In related research, platycodon extracts exhibit inflammatory modulating effects on human-cultured airway epithelial cells.19 Additionally, platycodon has been shown to modulate inflammation via diverse pathways, including IL-8 secretion by microglial cells.20
• Stemona (Bai Bu Radix Stemona) extracts display anti-tussive activity in a guinea pig cough model.21 In related research, stilbenoids, including resveratrol from Stemona root, inhibit leukotriene formation.22
• Licorice (Gan Cao, Radix Glycyrrhiza Uralensis) helps to modulate airway constriction, lung inflammation and infiltration of eosinophils in bronchial areas.23 In related research, glycyrrhiza root has been found to promote CD4 and CD8 immune cell function.24 A related study identifies the main anti-tussive active ingredients in glycyrrhiza root in various phases of the cough response.25
Addressing Cough
In describing his approach to cough, Dr. Fratkin emphasizes early action. Often, as the initial stages begin to set in many people take a wait-and-see approach, allowing symptoms to advance before considering serious treatment. According to Dr. Fratkin, this is a mistake, and the best thing to do is to take action at the first signs of discomfort. “In the early stages, before a cough has developed, I would actually use another product from Tango called ImmunoPhase. This formula contains very powerful botanicals used to support a healthy immune system response, including such herbs as Lonicera, Forsythia, Verbena, Ilex and Isatis. Coughs can be more stubborn, and the sooner they are addressed with BronchoPhase, the sooner they will resolve. In some cases this can take anywhere from three to twelve days, but with quick attention coughs will gradually lessen in both duration and severity.”BronchoPhase is appropriate for all ages including children above the age of six. For infants less than six years of age treatment with Chinese herbs should be given only by an experienced practitioner.
Image: Copyright Russell Knightley Media, Canberra, Australia.
References
1. Coon JT, Ernst E. Andrographis paniculata: a systematic review of safety and efficacy, Planta, 2004 Apr. Pubmed ID: 15095142.
2. Ko HC, Wei BL, Chiou WF. The effect of medicinal plants used in Chinese folk medicine on RANTES, Ethnopharmacol, 2006 Mar 17. Pubmed ID: 16621378.
3. Xia YF, Ye BQ, Li YD, Wang JG, He XY, Lin X, Yao X, Ma D, Slungaard A, Hebbel RP, Key NS, Geng JG. Andrographolide modulates inflammation by inhibition of NF-kappa B activation through covalent modification of reduced cysteine 62 of p50, Immunol. 2004 Sep 15. Pubmed ID: 15356172.
4. Sheeja K, Shihab PK, Kuttan G. Antioxidant and inflammatory modulating activities of the plant Andrographis paniculata Nees, Immunopharmacol Immunotoxicol. 2006. Pubmed ID: 16684672.
5. Yang ZC, Wang BC, Yang XS, Wang Q, Ran L. The synergistic activity with eight traditional Chinese medicines, Colloids Surf B Biointerfaces, 2005 Mar 25;41(2-3):79-81. Pubmed ID: 15737531.
6. Ma SC, Du J, But PP, Deng XL, Zhang YW, Ooi VE, XU HX, Lee SH, Lee SF. Chinese medicinal herbs, J Ethnopharmacol 2002 Feb, Pubmed ID: 11801383.
7. Huang Y, Tsang SY, Yao X, Chen ZY. Biological properties of baicalein in cardiovascular system, Curr Drug Targets Cardiovasc Haematol Disord, 2005 Apr;5(2):177-84. Pubmed ID: 15853750.
8. Kim EH, Shim B, Kang S, Jeong G, Lee JS, Chun M., Inflammatory Modulating Effects of Scutellaria baicalensis extract via Suppression of Immune Modulators and MAP kinase signaling molecules, J Ethnopharmacol. 2009 Aug 20. Pubmed ID: 19699788.
9. Lim BO., Effects of wogonin, wogonoside, and 3,5,7,2′,6′-pentahydroxyflavone on chemical mediator production in peritoneal exudate cells and immunoglobulin E of rat mesenteric lymph node lymphocytes, J Ethnopharmacol, 2003 Jan;84(1):23-9. Pubmed ID: 12499072.
10. Koo HJ, Lim KH, Jung HJ, Park EH. Evaluation of gardenia extract, geniposide and genipin, J Ethnopharmacol. 2006 Feb 20. Pubmed ID: 16169698.
11. Kang JJ, Wang HW, Liu TY, Chen YC, Ueng TH. Modulation of cytochrome P-450-dependent monooxygenases, glutathione and glutathione S-transferase in rat liver by geniposide from Gardenia jasminoides, Food Chem Toxicol., 1997 Oct-Nov. Pubmed ID: 9463529.
12. Chai OH, Lee MS, Han EH, Kim HT, Song CH., Morus Alba (Radicis Cortex Morus Alba) (Sang Bai Pi) Effects of Morus alba on compound 48/80 and anti-chicken gamma globulin IgE- mediated mast cell activation, Biol Pharm Bull, 2005 Oct, Pubmed ID: 16204934.
13. Kim HM, Han SB, Lee KH, Lee CW, Kim CY, Lee EJ, Huh H., Immunomodulating activity of a polysaccharide isolated from Mori Cortex Radicis, Arch Pharm Res,, 2000 Jan, Pubmed ID: 10896055,
14. Ahn KS, Noh EJ, Cha KH, Kim YS, Lim SS, Shin KH, Jung SH. Inhibitory effects of Irigenin from the rhizomes of Belamcanda chinensis on nitric oxide and prostaglandin E(2) production in murine macrophage RAW 264.7 cells, Life Sci., 2006 Apr 11;78(20):2336-42. Pubmed ID: 16307761.
15. Kim H, Lee E, Lim T, Jung J, Lyu Y., Modulating effect of Asparagus cochinchinensis on tumor necrosis factor-alpha secretion from astrocytes, Int J Immunopharmacol. 1998 Apr-May;20(4-5):153-62. Pubmed ID: 9730251.
16. Ozaki Y, Xing L, Satake M. Iinflammatory modulating effect of Trichosanthes kirilowii Maxim, and its effective parts, Biol Pharm Bull, 1996 Aug;19(8):1046-8. Pubmed ID: 8874813.
17. Chan SW, Li SL, Lin G, Li P., Pharmacokinetic study and determination of imperialine, the major bioactive component in antitussive Fritillaria cirrhosa, in rat by high-performance liquid chromatography coupled with evaporative light-scattering detector Anal Biochem. 2000 Oct 1;285(1):172-5. Pubmed ID: 10998280.
18. Shin CY, Lee WJ, Lee EB, Choi EY, Ko KH., Platycodin D and D3 increase airway mucin release in vivo and in vitro in rats and hamsters, Planta Med., Mar. Pubmed ID: 11914958.
19. Lee JH, Choi YH, Kang HS, Choi BT., An aqueous extract of Platycodi radix inhibits LPS-induced NF-kappaB nuclear translocation in human cultured airway epithelial cells, Int J Mol Med., 2004 Jun. Pubmed ID: 15138622.
20. Jang MH, Kim CJ, Kim EH, Kim MG, Leem KH, Kim J., Effects of Platycodon grandiflorum on lipopolysaccharide-stimulated production of prostaglandin E2, nitric oxide, and interleukin-8 in mouse microglial BV2 cells, J Med Food, 2006 Summer. Pubmed ID: 16822201.
21. Lin LG, Zhong QX, Cheng TY, Tang CP, Ke CQ, Lin G, Ye Y. Stemoninines from the roots of Stemona tuberosa, J Nat Prod., 2006 July. Pubmed ID: 16872143.
22. Adams, M, Pacher T, Greger H, Bauer R., Inhibition of leukotriene biosynthesis by stilbenoids from Stemona species, J Nat Prod., 2005 Jan. Pubmed ID: 15679323.
23. Ram A, Mabalirajan U, Das M, Bhattacharya I, Dinda AK, Gangal SV, Ghosh B. Glycyrrhizin, Int Immunopharmacol., 2006 Sept. Pubmed ID: 16846841.
24. Brush, Mendenhall E, Guggenheim A, Chan T, Connelly E, Soumyanath A, Buresh R, Barrett R, Zwickey H., The effect of Echinacea purpurea, Astragalus membranaceus and Glycyrrhiza glabra on CD69 expression and immune cell activation in humans, Phytother Res., 2006 Jun 28. Pubmed ID: 16807880.
25. Kamei J, Saitoh A, Asano T, Nakamura R, Ichiki H, Iiduka A, Kubo M., Pharmacokinetic and pharmacodynamic profiles of the antitussive principles of Glycyrrhizae radix (licorice), a main component of the Kampo preparation Bakumondo-to (Mai-men-dong-tang), Eur J Pharmacol, 2005 Jan 10. Pubmed ID: 15659306.


