Reversing Insulin Resistance to Reduce Type 2 Diabetes Leave a comment
While Regaining Control of Metabolism to Curb Carbohydrate Cravings, Control Weight
According to the New York Times, 800,000 New Yorkers – more than one adult in every eight – have diabetes. New York health authorities admit that “diabetes is a bona fide epidemic” and, in fact, the only major disease in the city that is growing, both in the number of new cases and the number of people it kills, even as other maladies like heart disease and cancers are stable or in decline.
Unfortunately, the crisis in New York City is mirrored by an unchecked epidemic of diabetes that is currently sweeping the United States. The situation has become so dire that the Centers for Disease Control and Prevention (CDC) is now predicting that one third of all children born in the US will become diabetic in their lifetime. For Latinos the forecast is even bleaker: one child in every two.
China has experienced a similar epidemic of diabetes that is blamed on the widespread adoption of a Western-style diet that is high in sugar, refined starches and processed foods. To address the problem Chinese medical researchers have developed a new herbal supplement, MetaPhase®, that is designed to support recovery from insulin resistance, the primary cause of obesity and obesity-related disorders such as diabetes.
By restoring healthy blood sugar regulation and normalizing insulin production, advanced herbal formulas have been shown to aid in reversing chronic metabolic and chemical disturbances caused by long-term exposure to elevated insulin and blood glucose levels. Additionally, by curbing carbohydrate cravings advanced herbal formulas have been shown to support safe and natural weight loss.
Diabetes occurs when blood sugar (glucose) accumulates in the bloodstream instead of being burned (metabolized) in cells for energy production. The result is that while cells literally starve for fuel, dangerously high levels of blood sugar course throughout the body causing widespread damage to tissues and organs. The resulting damage to the nervous system and circulation can lead to the amputation of toes, feet and legs; even a tiny cut on the foot can lead to gangrene because it is not seen or felt.
Diabetes primarily occurs in two versions. In Type 1, the immune system has destroyed the cells in the pancreas that produce insulin. Type 2 occurs when the body’s cells are not sufficiently receptive to insulin, or the pancreas makes too little of it, or both. Most Type 2 diabetics are typically over 40, overweight, and have the disease for seven to ten years before receiving a diagnosis. What is especially disturbing about the rapid rise of Type 2 diabetes, which accounts for an estimated 90 to 95 percent of all cases, is that it is largely a preventable disease.
Metabolic Syndrome
Metabolic syndrome, also referred to as insulin resistance syndrome or pre-diabetes, is the number one cause of Type 2 diabetes. According to the Journal of the American Medical Association (JAMA), metabolic syndrome has reached epidemic proportions, currently affecting one third of all men and women in the United States, or some 80 million adults. And in addition to being the leading cause of Type 2 diabetes, metabolic syndrome also contributes to increased incidence of heart attacks, stroke, cataracts and cancer.
First identified by Prof. Vladimir Dilman in the 1960s in his book, The Metabolic Pattern of Aging, and further elucidated by antiaging pioneer, Dr. Ward Dean in his groundbreakingNeuroendocrine Theory of Aging, wide-spread acceptance of the concept by the medical community didn’t occur until 1988. In that year Stanford University endocrinologist Dr. Gerald Reaven defined Syndrome X (later renamed Metabolic Syndrome) as a spectrum of related risk factors. Recently updated guidelines established by the National Cholesterol Education Program / Adult Treatment Panel III (NCEP/ATP III) in April 2005 call for a positive diagnosis of Metabolic Syndrome when three of the following risk factors are present:
- Obesity (particularly excess abdominal fat)
- Insulin resistance (glucose intolerance)
- Elevated LDL cholesterol and blood triglycerides
- Low HDL cholesterol
- Elevated blood pressure (120/80) or higher
- Inflammation (elevated C-reactive protein)
- Elevated fibrinogen levels (increased risks of thrombosis)
Metabolic syndrome doesn’t occur suddenly, but develops slowly over an extended period of time – 20 to 30 years in many cases. And while people may notice the obvious early symptoms, such as obesity, exhaustion, depression and increased carbohydrate cravings, most don’t realize they have metabolic syndrome until they are diagnosed with more serious medical conditions, such as hypertension, peripheral vascular disease or diabetes.
While the symptoms of metabolic syndrome are varied and often appear at different times, they all arise from the disruption of normal glucose metabolism.
Glucose and Energy Production
Human energy is derived from a simple sugar molecule called glucose. After a meal the body rapidly converts sugars and carbohydrates into glucose. As glucose levels rise in the blood stream the pancreas responds by secreting insulin, a specialized hormone that allows cells to absorb glucose and metabolize (burn) it to produce cellular energy.
When food intake exceeds the body’s energy requirements, the excess glucose is converted into glycogen, another type of sugar that is stored in the liver and muscle cells as a convenient short-term energy reserve. As energy demands rise and fall during the day the body converts glycogen back into glucose to stabilize blood sugar levels and maintain energy production. When food intake exceeds the body’s capacity to store glycogen, the excess is directed into long-term energy reserves in the form of fat.
Insulin Resistance
Insulin resistance occurs when cells become less sensitive to the effects of insulin. This results in rising blood sugar levels (hyperglycemia) and a drop in energy production. To compensate for insulin resistance – and to keep blood glucose levels from spiraling out of control – the pancreas tries to restore balance by producing more insulin. Left unchecked, cells become even more resistant to insulin even as the pancreas secretes ever greater amounts in a desperate attempt to bring the system back under control. This results in dangerously high blood levels of insulin (hyperinsulinemia). If not corrected the pancreas eventually becomes exhausted, resulting in diabetes and requiring daily blood monitoring and injections of insulin to manage blood sugar levels.
Metabolic Syndrome and Obesity
Insulin resistance and metabolic syndrome are closely linked to obesity, and both conditions are aggravated by a lack of exercise and a diet high in refined carbohydrates. Not surprisingly, many health experts believe that eating fewer carbs and increasing physical exercise will reverse metabolic syndrome and restore healthy glucose metabolism. This assumption is based on a simple equation: calories equal energy, and any energy not burned as fuel will be saved as fat. And therein lies a problem.
When applied to the unaltered chemistry of an otherwise healthy body, improved diet and exercise can aid in restoring healthy metabolic balance. But when the body is already in a state of chronic metabolic imbalance caused by long-term insulin resistance, such simple fixes often generate surprisingly different results.
How many times has someone said, “It’s my metabolism” when commenting on their weight, or talked about “starving” themselves while still putting on extra pounds? With insulin resistance even a small number of calories can result in obesity caused by an impaired ability to burn fuel and enhanced tendency to create and store new fat deposits.
Increasing Fat Storage with Carbs
Insulin resistance often triggers a sharp craving for carbohydrates, especially late in the evening. As cellular metabolism drops, energy levels plummet. This has a profound effect on the brain, which gobbles up 25 percent of the body’s available glucose reserves to support cognitive functions. When the brain is deprived of fuel mental performance is impaired, leading to fatigue, depression and more frequent headaches.
To improve mood and generate a quick lift many people reach for a bagel, a doughnut or some other refined carbohydrate to quickly elevate their blood sugar levels. Unfortunately this solution is only temporary and insulin quickly clears sugar from the blood stream. As sugar is converted into fat, energy levels plummet once again, triggering another round of intense carb cravings that can be impossible to resist.
As insulin resistance becomes more entrenched additional metabolic abnormalities begin to appear. Rising triglyceride levels act on muscle cells, further increasing their resistance to insulin and reducing their ability to burn fat. Triglycerides also affect adipose (fat) cells, making it increasingly difficult to release stored fat for energy production. Together the net effect acts like a one-way valve – fat is stored at an accelerated rate, but getting it out of storage becomes more difficult.
Suppressing Growth Hormone, Losing Lean Muscle Mass
Another side effect of elevated insulin levels is the suppression of growth hormone. Human growth hormone is normally released by the pituitary gland during the sleep cycle to aid in burning fat and rebuilding lean body tissues (muscles). Insulin exerts a direct and specific inhibitory effect on the release of growth hormone that disrupts the nightly regenerative cycle of tissue repair. In this way, elevated levels of insulin in the evening contribute to accelerated premature aging and reduced cellular metabolism, leading to further increases in body fat and loss of lean body mass. This explains why it is especially important for anyone trying to lose body fat to avoid late dinners and bedtime snacks.
“…even a small number of calories can result in obesity caused by impaired ability to burn fuel and enhanced tendency to create and store new fat deposits.”
Why Low-Carb Diets Fail
As the public was made aware of the link between carbohydrates and obesity, a number of new diets took over the weight-loss industry. Diets developed by Dr. Atkins, Barry Sears and others promote a sharp reduction in carbohydrate intake to 1) reduce insulin production and 2) increase the body’s ability to burn fat. Initially, many people found that they could forgo carbs for short periods of time and enjoy rapid reductions in body fat while improving blood lipid profiles. Unfortunately, low-carb diets failed to correct the entrenched metabolic problems caused by long-term insulin resistance. As a result many people discovered that low-carb diets are extremely difficult to maintain in the long-term.
The Link Between the Hypothalamus and Insulin
Much of the difficulty in maintaining a low-carb diet involves the body’s master gland – the hypothalamus. The hypothalamus is a key component of the limbic system, responsible for regulating hunger, thirst, body temperature and sleep cycles. Just as the pancreas keeps an eye on blood glucose and increases insulin production to bring sugar levels down, the hypothalamus monitors insulin and attempts to restore balance when levels are too high.
Since the best way to bring insulin down is to increase glucose, the hypothalamus responds to chronically elevated insulin levels by sending out signals – hunger pangs – to force the body to eat and thereby increase glucose levels. Given the number of abnormal signals coursing through the body, most people eventually surrender to the inexorable weight of the hypothalamus demanding food to offset the elevated insulin levels – and the quickest way to accomplish this is to ingest more carbohydrates.
Metabolic Syndrome and Weight Loss Supplements
Just as metabolic syndrome works against caloric- and carb-restricting diets, the presence of metabolic abnormalities also undermines the expected benefits of many weight-loss supplements. While it is easy to demonstrate that certain substances can enhance metabolism and speed up fat-burning in animal and laboratory settings, when unleashed upon a metabolic system already out of balance and on the verge of collapse, many products fail to deliver significant results. Why? Think of your car. If the tank is empty and the engine barely able to turn over, pouring fuel additives into the gas tank will not increase performance. At least not until the underlying issues are corrected.
Long-Term Health Complications
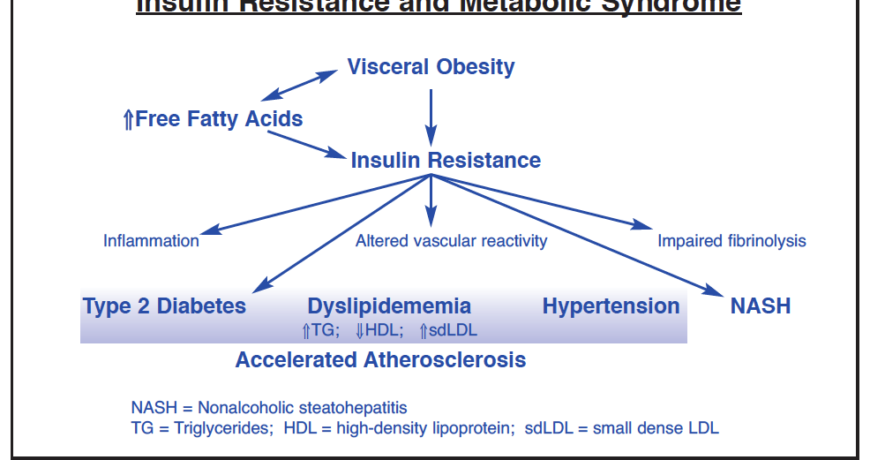
In addition to promoting obesity and diabetes, metabolic syndrome also causes metabolic changes associated with a number of chronic degenerative diseases. When insulin production is impaired, cellular energy levels plummet and biological functions are impaired. Additionally, excess glucose binds to proteins and cellular structures, causing damage to blood vessels, eyes, and other organs. For example, diabetics are five times more likely to develop cerebrovascular, peripheral vascular and coronary artery diseases than are non-diabetics. Glucose has also been shown to promote inflammation, a recognized risk factor for immune-related diseases and cancer. Additionally, by elevating blood levels of fatty acids, especially triglycerides, metabolic syndrome contributes to atherosclerosis and related vascular diseases (Fig. 1).
The Pharmacology of Metabolic Syndrome
Because metabolic syndrome develops over a long period of time many of the symptoms are diagnosed – and treated – as separate and unrelated conditions. Without identifying and correctly addressing the underlying condition, insulin resistance, many patients end up saddled with a wide range of treatments that can include statin drugs (to lower cholesterol), antidepressants (for depression and mood swings), ACE-inhibitors and beta-blockers (for hypertension) and anti-thrombolytic drugs (to reduce risk of developing blood clots).
Herbal Solution for Obesity and Insulin Resistance
In the 1980s doctors in China were alarmed by sharp increases in the incidence of diabetes, heart disease and breast cancer. Noting that these conditions were linked with the adoption of Western eating habits, Chinese doctors turned to Western drugs to treat the disorders. Eventually medical experts noticed that, in addition to having side effects, the drugs were failing to address the cause of the problems.
The central tenet of Chinese healing is to treat both acute symptoms and underlying causes of an illness. Based on this principal the Chinese researchers turned to traditional herbs that are well studied and widely used for diabetes. After almost ten years of clinical evaluation a team of doctors at Shanghai People’s Hospital developed MetaPhase, a unique herbal blend that effectively countered insulin resistance, lowered blood sugar levels and restored healthy pancreatic function.
In clinical tests these herbal ingredients were shown to restore health by countering the wide spectrum of disorders that accompany diabetes, such as cardiovascular disease, degenerative eye conditions, skin ulcerations, limb numbness and pain, and kidney dysfunction.
MetaPhase Ingredients / Actions |
|
Clinical Results with Humans
Case 1: Mr. S., 54-years-old, a Type 2 diabetic with fasting blood sugar of 335 mg/dl. Mr. S. was able to maintain fasting blood sugar levels of around 141 only by taking 18 units of insulin in the morning and 26 units in the evening. His doctor recommended MetaPhase, three capsules three times daily. After ten days, fasting blood sugar dropped to 124 and blood sugar two hours after eating fell to 141. Mr. S. subsequently discontinued insulin and after three months his fasting blood sugar has stabilized between 106 and 124.
Case 2: Mr. L., 56-years-old, presented with a fasting blood sugar level of 155 mg/dl. After 7 days on MetaPhase his fasting blood sugar was 101 and energy markedly improved. After three months he is still taking two capsules daily and fasting blood sugar stabilized between 97 and 106.
Case 3: Mr. L., 65-years-old, was taking insulin injections to maintain fasting blood sugar between 141 and 159 mg/dl, and blood sugar two hours after meals between 194 and 212. Mr. L. began taking MetaPhase, three capsules three times daily. In two weeks, his fasting blood sugar dropped to 115 and two hours after eating to 159. After using the formula for three months, his fasting blood sugar stabilized at 106 and remains stable.
Case 4: Mr. S., 35-years-old, with fasting blood sugar of 146 mg/dl. In April of 2004 he started taking MetaPhase, three capsules, three times a day. After 8 days his fasting blood sugar was 106. He was able to gradually decrease his medications and his blood sugar remains stable today.
MetaPhase and Weight Loss
In addition to normalizing glucose levels and restoring peripheral insulin sensitivity, MetaPhase has been shown to aid in helping with weight control. And unlike many formulas that elevate blood pressure, the herbs in MetaPhase have a history of restoring healthy blood pressure levels.
John, a 55-year-old executive, has experienced creeping weight gain over the years that he suspects was related to metabolic syndrome. After reaching a high weight of 184 pounds versus the 135 he weighed in high school, he went on the Atkins diet program and lost down to 160 pounds over a period of six months. Then his weight gradually went back up to 175, mainly because of carbohydrate snacking in the evening.
He attempted many times to restart the Atkins program, but felt thwarted by his carb urges. He also tried to start an exercise program, but stopped because it was leaving him exhausted.
John began taking MetaPhase, two capsules twice daily. He immediately noticed a reduction of appetite and regained his ability to control carb cravings, particularly at night. In the first month he lost 10 pounds, most noticeably around his lower abdomen, and experienced increase in energy and physical strength.
Using MetaPhase Herbal Formula
Based on clinical experience, we recommend taking two to three capsules of MetaPhase, two to three times daily, 30 minutes prior to meals. The combination of herbs in the formula will stimulate a steady improvement that becomes most noticeable in 7 to 10 days. Once blood sugar and insulin levels have returned to normal – usually within 1 to 3 months – switch to a daily maintenance program consisting of one capsule in the morning and one in the afternoon before meals to sustain optimal results.
Note: Type 2 Diabetics using MetaPhase to control blood sugar levels may also experience improvements in related morbidity factors, including hypertension, hyperlipidemia, nephropathy and neuropathy. People with these conditions should continue to be monitored by their physician for changes in their condition and modify medications as necessary.
Summary
MetaPhase herbal blend combines a blend of herbs that have been shown to support recovery from metabolic disturbances common to metabolic syndrome while repairing cellular damage caused by prolonged exposure to elevated blood sugar levels.